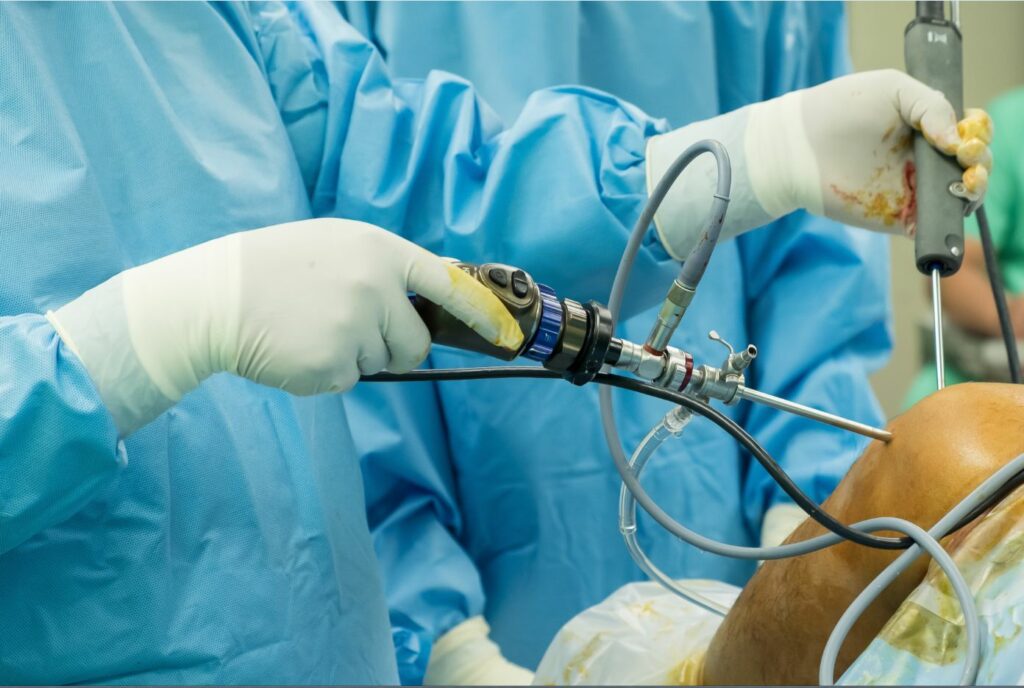
Knee Arthroscopy Vs Exercise for Osteoarthritis (OA)
The message is slowly filtering through the medical community and the general population that knee arthroscopy is no better than exercise for osteoarthritis (OA). More and more in my clinical practice I am coming across patients who are not surprised when I bring this up in our clinical sessions. Despite this, there are still tens of thousands of people who go through with a knee arthroscopy every year in Australia. A lot of them may even be aware of this information. This suggests that that some people understand the evidence but perhaps feel that they are different, perhaps it does not apply to them. This short blog will evaluate the arthroscopy research evidence, who it applies to, and potential harms associated with this surgery.
Interpreting the research
It is now well established that knee arthroscopy adds nothing in addition to exercise for knee osteoarthritis. But what does this mean? In the trials that have compared arthroscopy to exercise, both of the groups have been given similar exercise programs to complete, but one of the groups has also had an arthroscopy at the start. What the trials have found is that both groups have similar benefit for pain and function at the end of the trial, meaning that it is hard to say that the arthroscopy has done anything at all! Arthroscopy has also been tested in another way in clinical trials – against a placebo. In these trials, one group received a standard arthroscopy, the other group just had the incisions on their knee to make it look like they received the surgery. In these studies people who received the placebo surgery had similar benefit to people who had the arthroscopy.
The next question you might ask is,“Does this research apply to me?” A systematic review by Thorlund (2015) evaluated all the trials that have been performed on knee arthroscopy and compiled their results. The 9 trials included in the review tested arthroscopy on both sexes, ages ranging from 35-78, and OA ranging from mild to severe on imaging. On top of this, there were also 2 trials that included only people with meniscal tears, but no signs of OA. So, in summary if you are between 35 and 78, have any signs of OA or a meniscal tear, then this research directly applies to you.
Knee Arthroscopy Risks
All surgery, no matter how minimally invasive has risk. Some of these risks more serious than others. The same systematic review by Thorlund et al. (2015) outlined some of the risks of knee arthroscopy. They found that overall, adverse events occurred in about 14 cases per 1000. The most common adverse event was deep vein thrombosis (DVT) at 4.13 cases per 1000. This was followed by pulmonary embolism (blood clot in the lungs), infection, and death. Yes, people have died from routine knee scopes in research trials! A scary thought.
Cost Benefit Analysis – Arthroscopy vs Non-Surgical Management
Costs are another consideration when comparing treatment options for knee osteoarthritis. Marsh et al. (2016) analysed the costs and performed a cost benefit analysis between arthroscopy and non-surgical management for knee osteoarthritis. They cast the net wide in their analysis and not only included the direct costs of the surgery and exercise programs themselves, but also additional treatments that may have been used (medication, or injections), assistive devices, and days off work. On average, those in the arthroscopy group were out of pocket $1900 more than those in the non-surgical group. On top of this, the health system was also spending on average $2200 more on those in the arthroscopy group. They concluded that based on the outcomes and the associated costs, arthroscopy was definitely not an economically attractive treatment option!
Long term outcomes
Most research trials will follow up their participants for 12 months, or maybe 2 years at best. And in the trials looking at arthroscopy for knee OA, we know at this point in time both groups are returning similar results. But what happens after that? Brophy et al. 2014 looked at the trajectory of people following knee surgery to requiring a total knee replacement (TKR). They found that people who had undergone previous knee surgery were requiring TKR up to 10 years earlier than those who had not, suggesting that an insult to the knee such as surgery may even be a catalyst for the OA process.
In summary, if you are aged between 35 and 78, have a meniscal tear or signs of OA, then you may be better off seeking exercise-based care. You are likely to see similar benefit, spend less, expose yourself to less risks, and you may even prolong or eliminate the need for a joint replacement later on. Arthroscopy for knee OA really is “low value” care in every sense of the word. Minimal returns at a high price.